- News
- Reviews
- Bikes
- Accessories
- Accessories - misc
- Computer mounts
- Bags
- Bar ends
- Bike bags & cases
- Bottle cages
- Bottles
- Cameras
- Car racks
- Child seats
- Computers
- Glasses
- GPS units
- Helmets
- Lights - front
- Lights - rear
- Lights - sets
- Locks
- Mirrors
- Mudguards
- Racks
- Pumps & CO2 inflators
- Puncture kits
- Reflectives
- Smart watches
- Stands and racks
- Trailers
- Clothing
- Components
- Bar tape & grips
- Bottom brackets
- Brake & gear cables
- Brake & STI levers
- Brake pads & spares
- Brakes
- Cassettes & freewheels
- Chains
- Chainsets & chainrings
- Derailleurs - front
- Derailleurs - rear
- Forks
- Gear levers & shifters
- Groupsets
- Handlebars & extensions
- Headsets
- Hubs
- Inner tubes
- Pedals
- Quick releases & skewers
- Saddles
- Seatposts
- Stems
- Wheels
- Tyres
- Health, fitness and nutrition
- Tools and workshop
- Miscellaneous
- Tubeless valves
- Buyers Guides
- Features
- Forum
- Recommends
- Podcast
feature
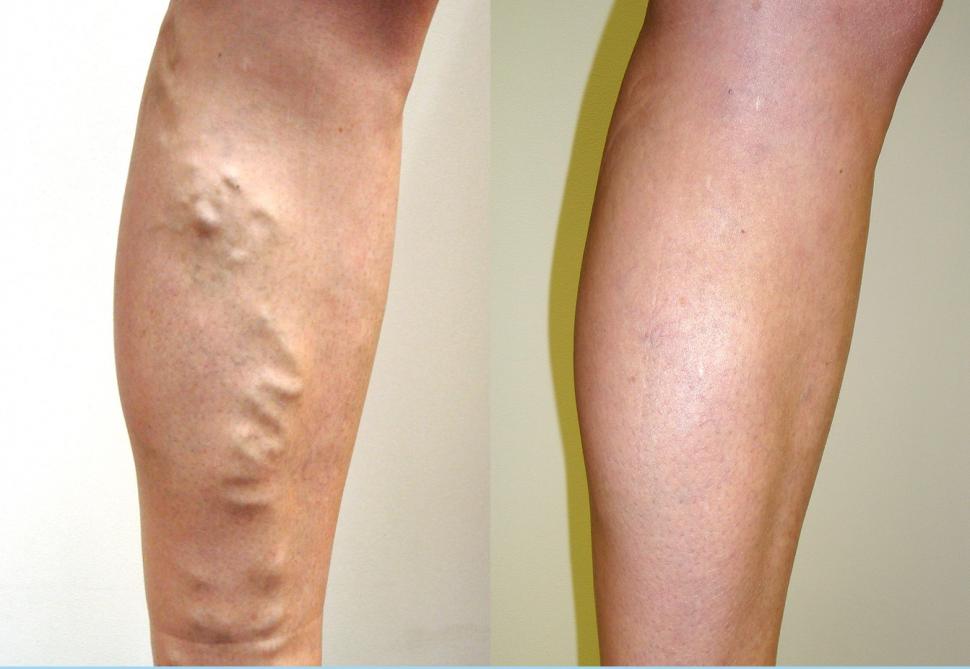
 Varicose veins in cyclists' legs
Varicose veins in cyclists' legsHealth Q&A: Varicose veins – why cyclists get them, and what you should do about them
First published August 6, 2020
Professor Mark Whiteley is one of the world’s leading experts in varicose veins. In this exclusive interview with road.cc’s Matt Lamy, he explains why cyclists seem to suffer more than most with the condition and what we should look for when it comes to treatment.
road.cc: First of all, what are varicose veins and what causes them?
Prof Whiteley: It’s important to understand that there’s a difference between a bulging vein that is normal but becomes apparent simply because you’re fit, and a varicose vein with an underlying cause, which is that the valves aren’t working and the blood is falling back down the leg rather than going back to the heart.
The problem we also have now with modern technology is that we find about 15% of the population have varicose veins that you can see on the surface, but there’s another 15% of the population where you see nothing on the surface at all, but the valves have gone in their veins underneath. These are the people who only realise they have varicose veins when they get swollen ankles, aching legs, skin damage, eczema, brown stains and eventually skin ulcers. In a book I wrote in 2011, I christened this phenomenon, ‘hidden varicose veins’.
How often do you treat cyclists?
I’ve been trying to do research on this for quite some time because we think that cyclists get a slightly different sort of varicose veins than normal people.
What one of my colleagues – Judy Holdstock, who is an expert in vascular technology – and I have noticed is that cyclists seem to have worse veins. We don’t know if that’s because cyclists are just slim and they’re using their legs a lot – so the venous return is high and they’ve got dilated veins because they’ve got a lot of blood flowing through them – or whether they’ve actually got varicose veins themselves. It’s quite a hard thing to tell just visually, because we’re seeing these veins in very fit people with low body fat.
However, when cyclists do come to see us, they seem to more commonly have a different sort of varicose vein, called a perforator vein. This is a really interesting condition because superficial veins should all take blood from under the skin, then perforator veins take the blood through the muscle – they perforate through the muscle – to the deep veins, and from there the blood shoots back up to the heart. There are about 150 perforator veins in the leg and if the valves go in those, what happens is that when you clench the muscle to drive the blood back to the heart it actually shoots out through the perforator veins.
Why do you think this happens?
What we think is happening is that, when cyclists put tremendous pressure across the calf muscles when they push the pedals, it causes huge pressure in the leg, which should push blood back to the heart. But sometimes that pressure – maybe if they’re hunched over and causing a temporary obstruction in the groin – might actually blow the valves out.
We have got some evidence for this. I wrote a study about one lady who came to see me and said she had been cycling up a hill when she felt like an elastic band had hit her leg. She looked down and saw there was a varicose vein. That was the first tangible proof we’d had that there is something behind our theory.
Is there anything that cyclists can do to prevent developing varicose veins?
The most important thing to say is that every single study that has ever been done on vein health and general health and exercise shows that the small problem of getting a varicose vein is completely dwarfed by the massive advantage to your health and your heart and your happiness and everything else by continuing to cycle. So the simple answer is, there’s almost nothing you can do to stop it, and it certainly shouldn’t put you off cycling because cycling is so good for all the other aspects of health.
Is any group of society particularly susceptible?
Yes – people whose mum or dad have varicose veins. Genetics is key.
Does having varicose veins affect cycling performance?
Not when cycling. The great thing we know about exercise is, because you’re creating such a lot of pressure at the bottom of your leg, all the blood is going back to your heart. So when you’re exercising, you’re actually reducing the risk of any complications.
The trouble is, you’re also dilating the veins so that when you’re off the bike sitting, resting or standing in normal life, that’s when the problems happen and you’ll start to get swelling of the ankle, brown stains, leg ulcers, etc. Being active helps delay the onset of complications – that’s been clearly proven. But the complications will still come if you don’t get your varicose veins fixed. It won’t affect your performance on the bike but it will affect your general health in time.
You mentioned earlier about hidden varicose veins – how would anybody know if they had a problem with those?
The things that will make you think you’ve got venous problems are aching legs, heavy legs, tired legs, cramps. Then, if you get to the next stage you can get swelling of the ankles, red stains or brown stains around the ankles, eczema, leg ulcers, even bleeding that is hard to stop if you prang one of the veins, clots, thrombosis or phlebitis.
So any of those things, from aching legs all the way through to any of those symptoms, any of those should get you to a proper venous surgeon or a phlebologist who will work in a team and get you a duplex scan by a proper vascular technologist. If a doctor tries to scan you themselves, walk out because they are not recognised to do that.
So it’s far more than just a cosmetic problem?
Absolutely, and this is why the NICE guidelines changed in 2013. I had been campaigning since 1999 to say the situation was ridiculous. Before 2013 people used to see varicose veins as just cosmetic whereas leg ulcers were serious. But varicose veins is actually a deteriorating condition: you start with some varicose veins, then more valves go, then you get swollen ankles and brown stains and eventually leg ulcers.
But if you treat varicose veins properly and early enough, you won’t get the problems later on. Unfortunately we seem to live in a society where people think varicose veins are just cosmetic and GPs aren’t educated in the newer vein problems. In the UK we don’t really have vein experts – there’s only about four of us – and most patients go to see a vascular surgeon instead, not realising that they are artery surgeons and none of those surgeons go to the big meetings where all of these new things are discussed.
We have a real problem in the UK where people with vein problems don’t get good care. There are a few opportunistic companies who are set up to treat people really quickly and cheaply, but people are getting terrible results and after a couple of years their veins are back again.
So what treatment options are there?
Treatment has actually changed a lot. Until 1999 everybody used to strip veins out – that was the standard treatment around the world. I was the first person to prove that you shouldn’t strip veins because they only grow back. Before that, no doctors would believe that the veins would grow back – although they would quite happily tell patients who had things like their gall bladders removed that the reason they healed was because the veins grew back! So no one should ever have their veins stripped, that’s the number one thing to understand.
Back in 1999 I introduced a new treatment where we burned veins. We previously used a radio frequency to do this but we discovered that is sub-optimal and have moved on to using lasers inside the veins. That is the industry standard. I’ve now moved on again to using microwave to heat the veins and shrivel them away – that is what I used on Chris Evans when he had his varicose veins done before Christmas. We’re trying to teach more people how to use that, although we are extremely short of vein specialists in the UK.
Is there anything potential patients should watch out for?
Some doctors are being incentivised to use Foam Sclerotherapy in every case of varicose veins. Unlike heat treatments, which instantly make the veins shrivel and die, Foam Sclerotherapy kills the vein but doesn’t shrivel it away – you have to do that with compression and must wear stockings and bandages for three weeks afterwards to keep the blood out of the veins. There are some doctors, especially in the Midlands, who are using Foam Sclerotherapy with every case of varicose veins. But the results of using Foam Sclerotherapy alone are poor because, although it works in small veins near the surface, the wall of bigger truncal veins is too thick and the foam can’t penetrate into it.
Instead, I follow the Whiteley Protocol, which we have developed over 25 years and uses a combination of other techniques such as Sonovein, laser or microwave for the deeper veins. Cyclists also have to make sure they have the perforators treated as well, otherwise there’s no point doing anything. Treatment is then done under local anaesthetic – it’s walk in, walk out, there’s no general anaesthetic or sedation. You go home, then eight weeks later you come back and we do the Foam Sclerotherapy for the smaller veins. That combination of treatments produces really good results with minimal pain and you can go straight back to work and exercise as normal.
And what does the future hold for varicose vein treatment?
The absolute latest technology I’ve mentioned is called Sonovein or High-Intensity Focused Ultrasound. What we do with that is put the ultrasound on the outside of the body and it beams a cone of ultrasound through the skin and burns the vein on the inside, so you don’t even get a cut. I did the first commercial case globally using this technology last year and we’ve now done 50 patients. I’ve also trained three other people to use it, because there are only three other machines in the world at the moment.
It’s early days but the results are looking really good. It’s absolutely space age stuff and what it will eventually lead to in 10 or 15 years when we’ve automated it all, is that you will go into your local chemist, put your leg in a box, pay with your credit card, and your varicose veins will be treated automatically.
Latest Comments
- eburtthebike 1 sec ago
Malicious: intended to harm or upset other people. Good luck proving that! How about pedestrians who are being malicious? Why only cyclists?
- lesterama 6 min 29 sec ago
Or go into his Swiss uncle's business
- hawkinspeter 42 min 57 sec ago
That's a plausible theory, but I suspect that the politics of oil consumption is a much bigger influence on the sentences given to protestors.
- Andski808 44 min 32 sec ago
Haven't seen the Revo but have seen Tubolito (similar price point) and I can't tell the difference between it and RideNow. Effectively both just...
- hawkinspeter 48 min 49 sec ago
So, what's next, taxing disabled people for any access ramps etc? How about taxing the drivers that end up parking on cycle lanes?
- Backladder 51 min 1 sec ago
Damn this labour government, they're going to tax VAT now, we should have listened to Rishi!
- Griff500 1 hour 31 min ago
Just to lighten the discussion a tad, this story brings to mind the case of Jed Singh Nagra, who several years ago named his convenience store on...
- Johnny Rags 1 hour 37 min ago
Ah, the Pedants' Revolt. Led, of course, by Which Tyler.
- eburtthebike 2 hours 7 min ago
No, the tunnel was not necessary and the congestion levels were self limiting. It's been repeated many times but is still beautifully apt:...

Add new comment
10 comments
I assumed varicose veins were just down to genetic predisposition, like teeth
All this talk of stripping veins is making me feel queasy.
I wonder whether cycling shorts with too much compression around the thigh, or over aggressive leg grippers, might play a part in constricting the venous flow leading to problems lower down the leg?
Interesting stuff. It would be beneficial if the interviewee's conflicts of interest were declared though, sounds like he has got commercial interests, which I have no problem with, but it might colour how I read some of his claims.
Indeed, some of this reads a bit like an advertorial.
I also wonder how to distinguish between the aching, heavy, tired, crampy legs I get from exercising hard and the same symptoms which mean I have a vein problem.
Brown stains on the lower calf do run in my family so I might want to get this checked - but my GP has got more on right now, so might not be all that keen on me wandering in with a bit of achy leg.
I agree there is something "off" about the tone of this piece. I was particularly disturbed by the last section where what looks like a highly experimental procedure is touted as "the future" on the basis of only 50 patients being treated, with no randomised controlled trial evidence to back it up (as far as I can see, only pilot studies are underway).
In essence, beware any doctor or surgeon who appears to be advertising in the Tatler magazine! He doesn't seem to work in the NHS so presumably relies on articles like this to drive his business...
https://www.tatler.com/article/professor-mark-whiteley-vein-doctor-london
It does kind of sound like "all other doctors are a bunch of charlatans, and I'm the only one who knows what I'm doing".
That was the feeling I got too...I mean, the guy might be speaking accurately but I'm always wary of "lone hero prepared to speak the truth" shtick which is laid on pretty heavily in this article.
That was the feeling that I got, too - although I was almost swayed by this revelation...
"In a book I wrote in 2011, I christened this phenomenon, ‘hidden varicose veins’. "
That must have taken a lot of expert consideration
Fascinating